Signs and symptoms
Do you have carpal tunnel syndrome?
What are the signs of carpal tunnel syndrome?
Carpal tunnel syndrome is fairly easy to diagnose. Your doctor will listen to you describe your symptoms and perform a complete physical examination of the affected hand or hands. They might perform additional tests to determine how severe it is and rule out other neuropathies or compression syndromes.

Diagnosis is based on your symptoms and a physical exam.
What tests are used to diagnose carpal tunnel?
There are several tests that can inform a carpal tunnel diagnosis. Certain positions and movements (referred to by doctors as maneuvers) are used to trigger symptoms, while others help gauge loss of feeling.
- Phalen’s maneuver: One test for diagnosing carpal tunnel is called Phalen’s maneuver. During the test, the patient maintains a forced 90-degree wrist extension for one minute. It can be more effective if they raise their hands over their head while maintaining the extended position. If the patient feels tingling in their index or middle fingers or has wrist pain, especially in both hands, it is very likely they have carpal tunnel syndrome. The maneuver can be done on both hands at the same time.
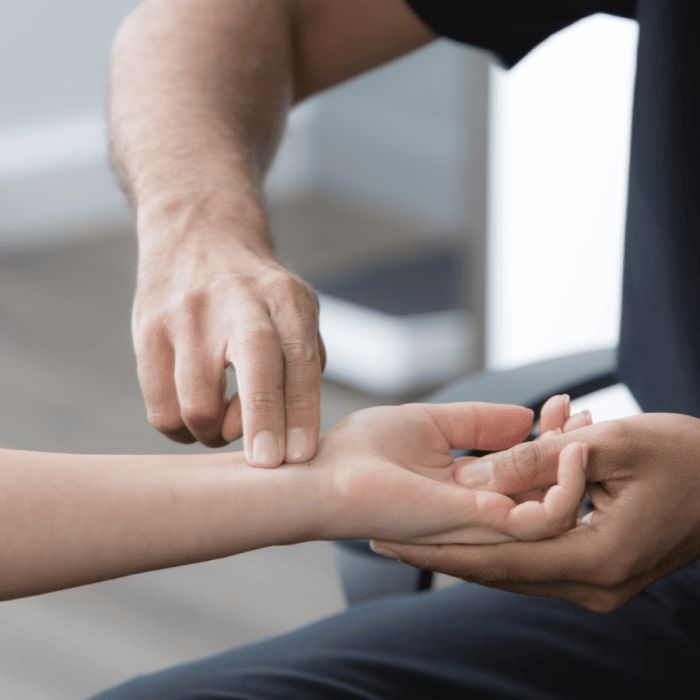
- Durkan’s test: Durkan’s test involves lightly compressing the median nerve using two fingers or the thumb at the forearm, about two to three centimetres above the carpal tunnel. If the test is positive, the compression will cause numbness or tingling in the fingers after about 20 seconds.
- Tinel’s sign: Tinel’s sign is a test that involves using two fingers to tap where the median nerve passes through the carpal tunnel. If the test is positive, this tapping will often cause a feeling like an electric shock or abnormal pain.
- Scratch collapse test: The Scratch Collapse Test is a useful physical examination maneuver for locating a second median nerve entrapment. The test involves comparing the resistance force of the lateral rotators by provoking (scratching) the inhibitory reflex of the suspected compression zone (inner face of the elbow). The test is considered positive and indicates the presence of lacertus syndrome if scratching induces a loss of strength. Surgical treatment must be adapted according to the diagnosis (isolated compression syndrome vs double crush syndrome).
- Sensitivity test: It can be helpful to compare the sensitivity of the ends (or pulp) of the index and middle fingers to that of the pinkie finger, since the pinkie is connected to a different nerve called the ulnar nerve. This sensitivity test can be done by gently touching the ends of the fingers with a cotton swab. If the level of sensitivity is different in the pinkie and ring fingers compared to the middle or index fingers, it’s likely the compression of the median nerve is already at a more advanced stage, pointing to a more severe condition that must be treated more urgently. This loss feeling can become permanent and debilitating.
Reproducing symptoms can help confirm a diagnosis


Ultrasound
Ultrasound is a technique your doctor can use to examine the median nerve and check its condition. If the nerve is compressed, it’s often wider right above the compression point. The nerve will appear bulged just before the area where it’s being pressed, like a garden hose that has a clog in it. With ultrasound, your doctor can find where the dilatation is and even measure the size of the nerve. It also helps identify where there are any anatomical abnormalities, like abnormal muscle, a growth in the tunnel, like a tumour or cyst, or a widening of the blood vessels.
Electromyography (EMG)
Electromyograms and nerve conduction velocities (how fast nerve signals travel) are very helpful and informative. These tests evaluate nerve function and performance, as opposed to imaging tests, which show how nerves look.
Nerves can be compared to big electrical cables containing hundreds of wires and cords (nerve fascicles, or bundles of nerve fibres).Nerve compression affects blood vessel formation and the supply of oxygen to the axons, which then start to malfunction. Conduction velocity, or how fast electrical signals travel through nerve fibres, decreases substantially. Electromyograms provide important insights into how advanced the condition is, as well as prognosis and recovery.
When patients are experiencing symptoms of early stage carpal tunnel syndrome, these tests can result in false negatives. If doctors or patients are unaware of the limits of these tests, the results can seem incorrectly reassuring and lead to delayed treatment.
MEET YOUR HAND EXPERT
A first step towards recovery
Carpal tunnel
syndrome severity
Carpal tunnel syndrome is classified into three stages depending on how severe symptoms are.
Stage 1 (Mild)
Patients with stage 1 carpal tunnel typically experience numbness, pain, and tingling, primarily at night, and can make the symptoms go away by shaking out their hands. Affected hands often feel stiff in the morning.
Stage 2 (Moderate)
Patients with stage 2 carpal tunnel also experience symptoms during the day, when their hands are in the same position for a long time, or while doing repetitive movements. Their hands often start to feel weak, and it’s not uncommon for them to drop objects they’re holding.
Stage 3 (Severe)
Patients with stage 3 carpal tunnel often experience atrophy, where the muscles connected to the median nerve permanently shrink. Because the nerve is injured and no longer sending signals to the brain, the tingling sensation might have gone away.
Other nerve compression syndromes
CTS symptoms can sometimes be confused with those of lacertus syndrome, the name for median nerve compression at the elbow. Any patient experiencing numbness in the parts of their hands that are connected to the median nerve (thumb, index and middle fingers) should be evaluated for both conditions.
Does carpal tunnel syndrome
have to be treated?
Key takeaways
_________________
What diagnostic tests are recommended?
In most cases, your doctor can diagnose carpal tunnel simply from hearing a description of your symptoms and performing a physical examination. Some tests may reveal how severe the condition is and help rule out other ones. For example, the scratch collapse test is useful for diagnosing nerve compression syndromes like CTS or lacertus syndrome.
Are imaging tests required?
Ultrasounds and electromyograms (EMGs) may be useful for determining how advanced the condition is and finding any other abnormalities or injuries.
Can I get carpal tunnel in both hands at the same time?
Carpal tunnel can frequently occur bilaterally, or in both hands at once. It can be symmetrical (equal intensity) or asymmetrical (different intensities).
Practical and comprehensive
medical guide
Everything you need to know to identify and treat Carpal tunnel syndrome. Written in clear and simple language by hand surgeon Dr. Jean-Paul Brutus, this e-guide identifies the causes, symptoms, and different ways to treat CTS and offers recommendations on how to ease your symptoms at home.


